A watershed for Veterans occurred in 1974 when ACC came into being. Veterans serving prior to 1974 are still covered by the old provisions, but those serving post 1974 are covered by the provisions of the Veteran Support Act 2014, provided that they have deployed on ‘operational service’ and any injury or illness develops on a deployment. The Ministerial Veteran’s Health Advisory Panel, (VHAP) established under the Veteran Support Act, are specifically charged with funding research on this ‘contemporary Veteran’ group, NZVA acknowledging that they ‘have had different experiences, and have different needs, compared with the older veterans. They are likely to have served in a number of deployments during their career, and come to us with more complex health issues.’
briefing to Hon Meka Whaitiri 2020
One of the ‘signature injuries’ of the wars in iraq and Afghanistan was post traumatic stress (PTS). The VHAP funded a study to look at this, but we invited all Veterans, because it is not just deployments that result in illness and injury.
We measured PTS using a questionnaire, The questionnaire included a measure of PTS (the Military Post-traumatic Stress Disorder Checklist; PCL-M), where scores ≥30 indicate the experience of significant PTS symptoms and scores ≥45 indicate a possible clinical diagnosis of PTS.
We had replies from 1817 Veterans. PCL-M scores were ≥30 for 549 (30%) participants and ≥45 for 179 (10%) participants. Factors associated with higher PCL-M scores were trauma exposure, older age, male sex, and Māori ethnicity. Factors associated with lower PCL-M scores were greater length of service, psychological flexibility, and better quality sleep. (This part of the questionnaire is just below so that you can see the symptoms.)
You will see that ‘avoidance’ (questions 6-7) and is a feature of PTS, which is why improving psychological flexibility by ‘taking action’ through a brief form of therapy ‘focussed action and commitment therapy’, FACT may help Veterans because thoughts are just that, thoughts. Poor sleep may well be a sign that all is not well.
PTS has been studied a lot, but wellness in Veterans has not, so we asked the same group to rate, on a score of 0-100, where 0 is the worst health that you can imagine, and 100 is the best health that you can imagine, how you feel today.
The results were the opposite: length of service, deployment, psychological flexibility and better sleep quality were associated with higher EQ-VAS scores; age and distress with lower EQ-VAS scores.
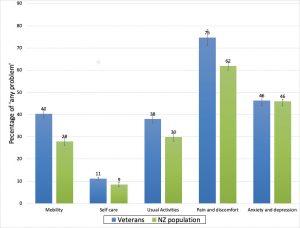
We also asked about problems with mobility, self care, usual activities, pain and discomfort and anxiety or depression. Veterans had more problems in the first three.
The reason why, and it may be just coincidence, is that lower limb injuries are a problem.
The commonest lower limb musculoskeletal injuries in a study that we did were ankle sprains or strains (35%) and knee sprains or strains (16%). Most commonly, injuries were due to acute over-exertion (37%), involved no other person (50%), and occurred while running (28%) or playing team sports (25%). The injury rate for recruits was more than five times that of trained personnel.
We thought that potential interventions should have targeted ankle sprains primarily,
but also knee sprains and fractures. Fractures, while accounting for only 6%
of lower limb injuries, should be a priority because of their high medical and time- lost costs.
Lower limb injuries descriptive
Last but not least there is stoicism, an ancient greek philosophical thing about how much you could harden up, but one of our Veteran participants gave us the line ‘soldiering on only goes so far.’
You can see the rest here:
It might improve your French.
Kia mate toa,
Dave